Appointment Timing - 9am to 6pm
What’s Wrong With My Pancreas?
Acute Pancreatitis
This is a patient information booklet detailing practical information about pancreas in general & specific information about acute pancreatitis. Its aim is to provide the patient & his or her family with useful information on this particular pancreatic problem, the procedures and tests you may need to undergo, various treatment approaches available with risks involved and helpful advice on coping successfully with the problem. If you require any further information or advice or are unsure about anything, Dr. D.R.Kulkarni or your own doctor will be able to help
In this Article
- What Is Pancreas?
- What Does The Pancreas Do?
- What Happens To Pancreatic Function In Pancreatic Diseases?
- Which Are Common Diseases Of Pancreas?
- What Special Investigations Are Done When A Problem Is Suspected With The Pancreas?
- Acute Pancreatitis
- What Is Acute Pancreatitis?
- What Happens In Acute Pancreatitis?
- What Is The Risk Of Complications And Death Following Pancreatitis?
- What Are The Long Term Effects Of Acute Pancreatitis?
- What Is Recurrent Acute Pancreatitis (Rap)?
- What Causes Acute Pancreatitis?
- What Causes Acute Pancreatitis In Children?
- GALLSTONES (Biliary Pancreatitis)
- How Do Gallstones Cause Pancreatitis?
- What Is The Treatment For Gallstone Pancreatitis?
- Who Can Develop Alcoholic Pancreatitis?
- How Does Alcohol Cause Pancreatitis?
- Severe Pancreatitis And Its Complications
- What Are The Symptoms & Signs Of Acute Pancreatitis?
- How Is Severe Pancreatitis Treated?
- What Are Complications Of Pancreatitis?
- Living Without A Pancreas
- Doctors Dealing With Pancreatic Disease That You May Meet
What Is Pancreas?
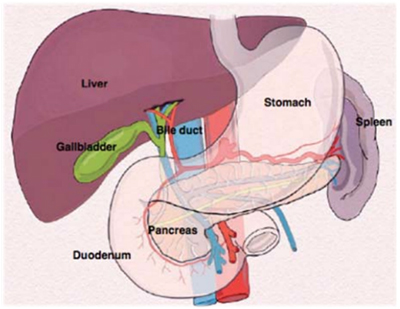
The pancreas is a solid gland attached in the back of the abdominal cavity behind the stomach. The pancreas is divided into 5 parts - the head, the uncinate process, the neck, the body and the tail. The head of the gland is closely attached to the duodenum which is the first part of the small intestine into which the stomach empties liquids and partially digested food. The head of the gland is situated just to the right of the midline of the abdomen and below the right ribcage. The uncinate process is an extension of the lower part of the head of the gland, which surrounds important blood vessels. The body and tail of the pancreas lie at an angle so that the tail of the pancreas is situated beneath the extreme edge of the left rib cage. The tail of the gland is closely attached to the central part of the spleen & splenic blood vessels.
Running behind the neck and uncinate process are many important blood vessels which supply the liver, the rest of the gut organs and the kidneys, including the aorta (an artery) which takes all the blood to the lower abdomen and legs, and the inferior vena cava (a vein) which returns blood from these areas. The splenic vein runs immediately under the tail and body of the pancreas and joins with the portal vein that runs immediately under the neck of the pancreas.
In short, pancreas is a centrally located and very precariously connected to or is in very close contact with most of the important structures in the abdomen. Hence diseases affecting pancreas can inadvertently involve any one or more of these structures. Hence patients with pancreatic problems may not necessarily have pancreatic complaints, but can present with unrelated complaints.
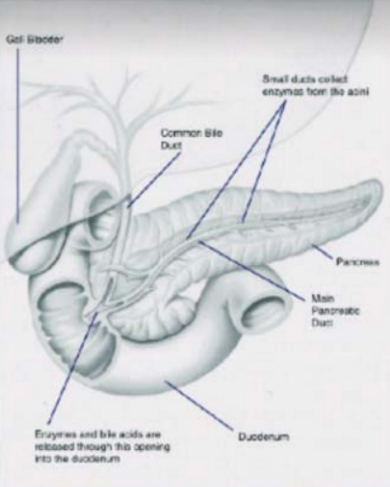
Running along the length of the pancreas within its centre is the main pancreatic duct, which empties pancreatic juice into the duodenum. Also running through the middle of the head of the pancreas is the main bile duct which also empties into the duodenum. (The main bile duct carries bile from the liver where it is made and also from the gallbladder where it is stored). In most people the pancreatic duct and bile duct join together just before they open into the duodenum through a large fleshy nipple called the ampulla of Vater (after the person who described this).
Surrounding the openings of each of these ducts are small muscles that control the release of pancreatic juice and bile and thus act as valves (also called sphincters). There is also a valve that regulates the pancreatic juice and bile together and this sits in the ampulla. This common valve is called the sphincter of Oddi, also named after the man who described this.
About one in ten people have two separate pancreatic ducts, one that opens as normal through the ampulla of Vater and the other through a smaller nipple (called as papilla). For this reason the ampulla of Vater is sometimes called the major papilla and the other smaller opening is called the minor papilla. The pancreatic duct that opens through the minor papilla is called the accessory pancreatic duct (normally this joins the main pancreatic duct rather than opening separately into the duodenum).
What Does The Pancreas Do?
The pancreas does two important things:
1) It makes enzymes which are necessary to digest food in the intestines.
Food consists of carbohydrates (e.g. glucose), proteins (e.g. meat) and fat (e.g. butter). Pancreas secretes different enzymes, which are responsible for breaking down clumps of different types of food into small particles for absorption. (Process of digestion) The main enzymes include amylase for digesting carbohydrates, trypsin for digesting proteins and lipase for digesting fats.
These enzymes are collected from the small glands in the pancreas into small ducts and finally into the main pancreatic duct to be released into the duodenum. The enzymes when they are first made in the acini are not active (otherwise they would digest the pancreas as well!). When they pass into the duodenum however, they are made active by the juice of the duodenum.
If there are not enough pancreatic enzymes, fat is not digested and the stools (bowel motions) become pale and greasy. These greasy stools may become difficult to flush away from the toilet and may give off a strong offensive smell. Doctors call this steatorrhoea (fatty stool.)
The digestion of fat is very special. Fat needs to be dispersed before the pancreatic enzymes can properly break it down. This dispersion of fats is made by bile acids which are present in bile produced by the liver and stored in the gall bladder. Bile acids act in exactly the same way as detergents, which are used to wash up greasy dishes. Therefore, both bile acids and pancreatic enzymes are needed for fat digestion. If the main bile duct becomes blocked, then the bile cannot get into the duodenum & fat cannot be properly digested.
When this common opening is blocked, the bile made by the liver cannot go into the bowel it goes into the blood and out through the kidneys into the urine. This results in the eyes and skin becoming yellow and is known as jaundice. As the bile is in the urine this now becomes dark in color. Because the flow of bile is blocked (or obstructed), doctors call this condition obstructive jaundice. As the bile duct goes through the head of the pancreas, jaundice can be caused by disease of the pancreas (such as pancreatitis or cancer).
2) It produces insulin to enable every part of the body to use glucose (sugar)
Insulin is a hormone made in special groups of cells called islets of Langerhans, which are dispersed throughout the pancreatic gland. It helps the cells of the body to use glucose as a source of energy in order to maintain their different functions. In absence of insulin, sugar instead of entering the cells of the body, stays in the blood leading to harmfully high concentrations. (Diabetes mellitus)
A large proportion of the islets (pronounced 'eye-lets') are in the tail of the gland. Most of the pancreas can be removed but there are usually enough islets remaining to make insulin sufficient to prevent sugar diabetes from occurring.
As you are probably aware, diabetes can be treated by taking regular injections of insulin, which can be taken from the pancreas of animals (e.g. pork insulin) or made by genetic engineering (so called 'human' insulin).
What Happens To Pancreatic Function In Pancreatic Diseases?
If pancreatic duct outflow is blocked due to any reason, gradually pancreatic duct enlarges in any size due to backpressure. Eventually the increased pressure within the duct starts taking toll on the pancreatic enzyme secretion, which drops and affects the digestion of food and absorption of nutrients, thereby affecting a persons weight and overall health. The insulin production is not immediately affected but over a period it will also drop thereby causing sugar diabetes in the patient.
Enzyme production and insulin production are independent. Because digestive enzymes and insulin are made by different parts of the pancreas, a problem with enzyme production does not mean necessarily that there will be a problem with insulin production. Similarly, if there is a problem with insulin production, this does not mean necessarily that there will be a problem with enzyme production. Assuming that the pancreas was normal to begin with, increasing loss of the pancreas gland (by disease or surgery) usually results in more loss of enzyme production before there is obvious loss of insulin production. Another way of saying this is that the insulin 'reserve' is much more than the enzyme 'reserve' of the pancreas.
Which Are Common Diseases Of Pancreas?
- Acute Pancreatitis
- Chronic Pancreatitis
- Pseudocyst
- Pancreatic fistula
- Cancer of pancreas
- Cystic tumors
- Neuroendocrine tumors
What Special Investigations Are Done When A Problem Is Suspected With The Pancreas?
You may need to do some tests to find out more about your particular problem. Perhaps you’ve already undergone one or more of them.
You may be advised to have certain blood tests like complete blood count, blood urea, creatinine, liver function tests (bilirubin, liver enzymes like SGOT, SGPT, Alkaline phosphatase, gamma GT, albumin), amylase, lipase, calcium, and parathormone. In case of acute pancreatic problems you will be advised to get admitted and all these tests will then be done in-house. Similarly diagnosis of pancreatic problems requires radiological imaging studies of abdomen like Ultrasonography, CT scan, MRI or further interventions like gastrointestinal endoscopy, ERCP, PTHC or EUS. It quite often so happens that patient is advised these investigations in a sequential manner and not at one go. This does take time but considering the cost of these investigations it is always better to ask for the next investigation only if it is absolutely necessary. Unfortunately in a small group of patients one cannot reach a diagnosis in spite of all this effort.
Acute Pancreatitis
This section deals with the particular problem you may have with your pancreas – “acute pancreatitis”. So what is it, what causes it, and how can it be treated?
What Is Acute Pancreatitis?
This is an inflammation & swelling of the pancreas which develops very suddenly and, in the majority of patients (about 75%) improves steadily with good in hospital treatment over the course of a week or so.
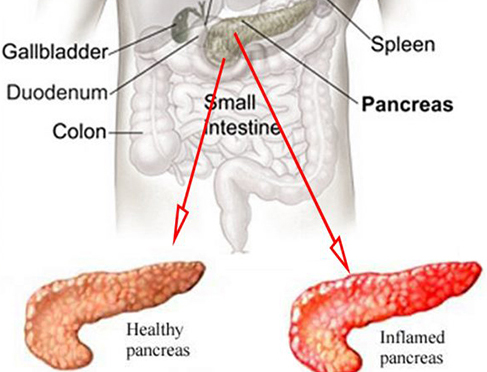
Yes, it requires a certain hospitalisation
A blood sample usually shows the presence of a large amount of amylase & lipase (pancreatic enzymes) in the blood.
What Happens In Acute Pancreatitis?
The pancreas produces chemicals called enzymes, as well as the hormones insulin and glucagon. Most of the time, the enzymes are only active after they reach the small intestine, where they are needed to digest food. Because premature activation of pancreatic enzymes within the pancreas leads to organ injury and pancreatitis, several mechanisms exist to limit this occurrence.
Under various conditions, these protective mechanisms are disrupted & enzymes somehow become active inside the pancreas, they eat (and digest) the tissue of the pancreas. This causes swelling of the pancreas, collection of fluid in surrounding areas & also in distant tissues, bleeding (hemorrhage); and damage to the pancreas and its blood vessels with eventually death or gangrene of pancreatic tissue (pancreatic necrosis).
As the toxins spread in the body, complications can arise in the rest of the body as well, such as microorganisms enter bloodstream through the porous intestinal walls, breathlessness (Acute Respiratory Distress Syndrome -- ARDS) or respiratory failure due to accumulation of fluid in lungs (wet lungs) & around lungs (pleural effusion), gastrointestinal bleeding and renal failure.
The inflammatory process initiated by pancreatitis can involve the entire body if very severe & is called Systemic Inflammatory Response Syndrome (SIRS) it can lead to the development of systemic shock. Eventually, the inflammation can become so overwhelming to the body that hemodynamic instability and death ensue.
What Is The Risk Of Complications And Death Following Pancreatitis?
The overall risk of death of patients with acute pancreatitis is 10-15%. About 20% of pancreatitis attacks are severe with associated pancreatic necrosis or some or other organ failure and chances of various complications are high in these patients. In patients with necrosis without organ failure, the mortality or death rate approaches zero. However in patients with severe disease (organ failure), the death rate is approximately 30%. This rate in mortality has not dropped in the last 10 years. In the first week of illness, most deaths result from multiple organ system failure. In subsequent weeks, infection plays a more significant role, but organ failure still constitutes a major cause of mortality.
Patients with biliary pancreatitis (caused by gall stones) tend to have a higher mortality rate than patients with alcoholic pancreatitis (caused by alcohol consumption). This rate has been falling over the last two decades as improvements in supportive care have been initiated.
What Are The Long Term Effects Of Acute Pancreatitis?
Usually after a regular mild attack of acute pancreatitis settles, the function remains unaffected. Once a patient has recovered from an attack of acute pancreatitis, they are perfectly well and there is usually no permanent damage to the pancreas.
However there are always exceptions to this rule. When the attack is very severe and causes death of pancreatic tissue, the function certainly gets affected. Similarly if there are repeated acute attacks then function can get affected over a period as chronic pancreatitis sets in. Therefore it is very important to find out the cause of acute pancreatitis, which must then be dealt with otherwise further attacks may follow. However cases of recurrent acute pancreatitis are few.
What Is Recurrent Acute Pancreatitis (Rap)?
If more than one attack of acute pancreatitis occurs, it is called recurrent acute pancreatitis.
What Causes Acute Pancreatitis?
There are many causes of acute pancreatitis, and it can affect people of any age. Men are affected more often than women.
Alcoholism and gallstones most often cause the condition. Genetic changes may be a factor in some cases. Sometimes the cause is not known, however (termed idiopathic). In 10-30% of cases, the cause is unknown in the initial investigations, but persistent investigations are able to solve the dilemma in almost 70% of these.
The etiology in males is more often related to alcohol; in females, to biliary tract disease. Idiopathic pancreatitis has no clear predilection for either sex.
Other conditions that have been linked to pancreatitis are:
- Autoimmune problems (when the immune system attacks the body)
- Blockage of the pancreatic duct or common bile duct, the tubes that drain enzymes from the pancreas
- Damage to the ducts or pancreas during surgery
- High blood levels of fat called triglycerides (hypertriglyceridemia)
- Injury (Trauma) to the pancreas from an accident
- Pancreas divisum (congenital anatomical problem)
- Annular pancreas (congenital anatomical problem)
- Choledocal cyst (congenital anatomical problem)
- Abnormal joining of pancreatic & bile duct (congenital anatomical problem)
- Pregnancy
- Heredity or genetic problems
- High blood calcium levels (hypercalcemia)
- High parathyroid hormone levels due to any cause (hyperparathyroidism)
- Drugs (e.g. estrogens, corticosteroids, thiazide diuretics, and azathioprine)
- Viral infections like mumps
What Causes Acute Pancreatitis In Children?
In children acute pancreatitis is usually due to gallstones, trauma, medicines, viral infections, genetic issues or congenital anatomical problems.
GALLSTONES (Biliary Pancreatitis)
This is by far the commonest cause of acute pancreatitis. Because gallstones affect women more commonly than men, acute pancreatitis usually affects women and even teenagers. Not all patients with known gallstones however develop acute pancreatitis – the figure is about 1 in 15 only.
How Do Gallstones Cause Pancreatitis?
Gallstones cause acute pancreatitis because they pass into the bile duct and temporarily block the opening into the duodenum at the point where it is joined by the pancreatic duct. The risk of a stone causing pancreatitis is inversely proportional to its size. Large stones find it difficult to slip down into the bile duct. Unknown microlithiasis (very minute stones or stone sand or crystals) is probably responsible for most cases of idiopathic acute pancreatitis.
What Is The Treatment For Gallstone Pancreatitis?
Once symptoms have improved the best way to prevent further attacks of acute pancreatitis is to have the gallbladder removed ('cholecystectomy’). This operation is now done best by keyhole surgery – so called laparoscopic cholecystectomy or ‘lap chole’ – under a general anesthetic. (Misnomer—laser cholecystectomy or laser surgery)
In severe cases, patients may benefit from an emergency endoscopy and cutting the lower end of the bile duct. This cutting is called ‘endoscopic sphincterotomy’. It makes the opening of the lower bile duct bigger, which allows any stones to pass through into the duodenum without causing blockage.
Elderly patients may not be suitable for a general anesthetic. An alternative then to a ‘lap-chole’ is endoscopic sphincterotomy. It causes complications in about 10% of cases and very occasionally a patient dies as a result. This risk is worth taking in an elderly patient who cannot have a ‘lap-chole’. On the other hand in younger patients a ‘lap-chole’ is safe & compared to that the risk of endoscopic sphincterotomy complications may be too high. Endoscopic sphincterotomy doesn’t avoid other gall stone-related complications like cholecystitis (inflammation of gall bladder), pus formation (empyema) or obstruction of bile duct with large stones.
ALCOHOL
This is the second commonest cause of acute pancreatitis overall although in some countries, it is perhaps a commoner cause than gallstones (USA).
Who Can Develop Alcoholic Pancreatitis?
Most commonly, the disease develops in patients whose alcohol ingestion is habitual over 5-15 years. Alcoholics are usually admitted with an acute exacerbation of chronic pancreatitis. Occasionally, however, acute pancreatitis can develop in a patient with a weekend binging habit, or a sole large alcohol load can precipitate a first attack. Nevertheless, the alcoholic who imbibes routinely remains the rule rather than the exception.
How Does Alcohol Cause Pancreatitis?
It is not known how alcohol causes acute pancreatitis, though many theories are postulated. Also, there is no universally accepted explanation for why certain alcoholics are more predisposed to developing acute pancreatitis than others who ingest similar quantities. Suffice to say some people have a pancreas, which is more sensitive to the effects of alcohol. These people develop attacks of acute pancreatitis a few hours or 1-2 days after they have been drinking alcohol. Often the sensitivity only develops after they have been drinking for several years. Such people may only be drinking a moderate amount of alcohol (not ‘heavy’ drinkers) and have actually developed chronic pancreatitis, which leads to intermittent acute attacks.
Other people who are much heavier drinkers may never develop acute pancreatitis but instead develop liver cirrhosis. Some patients who drink alcohol in moderate amounts never develop either acute pancreatitis or liver cirrhosis.
Is It Mandatory To Stop Alcohol For Patients With Alcoholic Pancreatitis?
If alcohol is the cause of your acute pancreatitis, it is essential that you stop all future alcohol drinking. Non- alcoholic drinks mimicking wine or beer are now reasonable substitutes. Low-alcoholic (LA) drinks should also be avoided however.
Hyperlipidaemia
This refers to an excessive level of lipids (particles of fat) in the blood. Lipids are essential to life and need to be transported by the blood from one tissue to another. Certain individuals have unusually high lipid levels in the blood and this can cause acute pancreatitis. Patients who drink a large amount of alcohol can also develop hyperlipidemia.
Which Lipids Are Responsible For Acute Pancreatitis?
Not all lipids are the same and it is only a certain pattern of lipids, which is associated with acute pancreatitis. For example, individuals who have a high blood cholesterol level are predisposed to heart disease and a high blood pressure but are not usually predisposed to developing acute pancreatitis. But high levels of triglycerides can lead to pancreatitis. Clinically significant pancreatitis usually does not occur until a person's serum triglyceride level reaches 1000 mg/dL. It is associated with type I and type V hyperlipidemia.
Hyperlipidemia is not a common cause of acute pancreatitis – it accounts for no more than 1% of cases. This type of pancreatitis tends to be more severe than alcohol- or gallstone-induced disease. The diagnosis is made by measuring blood lipid levels at the time of an attack of acute pancreatitis. At other times, the blood lipid levels may be normal. Treatment involves adopting a low fat diet. Occasionally special drugs need to be taken which can lower the level of abnormal lipids in the blood.
Narrowing Of The Pancreatic Duct
There are many different reasons why the pancreatic duct becomes narrowed like inflammation, stone, tumor, previous acute attacks, immune system disorders (autoimmune), previous surgery or trauma. For this reason, it is important not only to show that the pancreatic duct is narrow but also the cause for this. Surgery is often required to deal with pancreatic duct narrowing.
Pancreas Divisum
The pancreas develops as two separate buds from the intestinal tube during embryological development of the fetus in the womb. These buds each have a separate pancreatic duct. The two buds eventually combine together before birth to form a solid single organ. When this occurs, the separate pancreatic ducts also combine. In about 10% of healthy individuals, the pancreatic tissue combines but the two pancreatic ducts remain divided and they empty separately into the duodenum. This situation is called pancreas divisum because the pancreatic ducts remain divided.
Pancreas divisum is not harmful in the vast majority of cases. Very occasionally one of the ducts becomes narrowed and this can result in recurrent attacks of acute pancreatitis. Sometimes this may eventually lead to chronic (or continuous) pancreatitis. Although controversial, the presence of stenotic minor papillae and accessory pancreatic duct are additional risk factors that together contribute to the development of acute pancreatitis through an obstructive mechanism.
The treatment involves enlarging the narrowed pancreatic duct opening and can be done endoscopically (endoscopic sphincterotomy). Previously an open operation used to be performed for the same purpose that involves opening the duodenum (trans-duodenal sphincteroplasty). The operation enlarges both the biliary and pancreatic sphincters. With availability of endoscopic skills it is rarely done now.
If the pancreatic duct is very distended then this can be drained into a piece of bowel and the operation is called a pancreato-jejunostomy. If the head of the pancreas is damaged by the pancreatitis sometimes it may be necessary to remove a part of the pancreas ((Beger’s operation/Frey operation/head coring).
Annular Pancreas
This is an extremely rare cause of acute pancreatitis which often affects small children but which can affect adults. The problem arises during embryological development of the two pancreatic buds as described above (see pancreas divisum). In simple terms, the head of the pancreas becomes partly or totally wrapped around the duodenum (beginning of small intestine). This can cause an obstruction to the flow of food in very young babies & is relieved by operation called duodeno- duodenostomy.
Alternatively the flow of pancreatic juice along the pancreatic duct may be hindered leading to acute pancreatitis. This may be difficult to recognize but once it is, surgery is required. The type of surgery will depend on the exact nature of the pancreatic duct blockage.
Sphincter Of Oddi Dysfunction (SOD)
There is a valve in ampulla that regulates flow of pancreatic juice and bile together. This common valve is called the sphincter of Oddi. Abnormal pressures in this valve due to malfunction can lead to acute pancreatitis by causing increased pancreatic ductal pressures.
Trauma (1.5%)
Any major blunt injury to the abdomen may cause acute pancreatitis. Blunt injury may crush the gland leading to injury.
Post-ERCP (4%)
Post-ERCP pancreatitis is probably the third most common cause of pancreatitis. The risk is increased if the endoscopist is inexperienced, the patient is thought to have sphincter of Oddi dysfunction (SOD), or manometry is performed on the sphincter of Oddi.
Surgery
This is also another rare cause of acute pancreatitis. Surgery performed to organs which lie near the pancreas such as the stomach, spleen or kidneys can cause acute pancreatitis. For reasons we do not understand, surgery to organs well away from the pancreas (such as the prostate gland, heart and brain) can also cause acute pancreatitis. Postoperative acute pancreatitis is often a difficult diagnosis to confirm, and it has a higher complication rate than pancreatitis associated with other etiologies.
Autoimmune Pancreatitis
This is a rare condition that causes acute pancreatitis. The actual cause of the condition is not known. In the pancreas of this condition there are many cells of the type that make antibodies and other cells involved with immunity. This is why it is called autoimmune pancreatitis. It is like one’s own immune system active against its organs.
The diagnosis is extremely difficult to make. t requires high degree of clinical suspicion accompanied by special blood tests (level of special antibodies called IgG4 in blood), radiological imaging (CT scan) and biopsy of pancreas.
It is usually in young people (approximately 40 y) who also suffer from inflammatory bowel disease. There is often obstructive jaundice and a swelling in the head of the pancreas. It is therefore not surprising that it is often confused with chronic pancreatitis or a tumor in the head of the pancreas. In fact the correct diagnosis is usually only made after major surgery to remove the head of the pancreas (Whipple operation). The condition will respond to a course of steroids and pancreas enzyme supplements.
Pregnancy
A small number of women develop acute pancreatitis during pregnancy. The cause is not the pregnancy itself but another underlying reason. Investigation nearly always shows that the cause is gallstones because in some women pregnancy speeds-up the development of gallstones due to the increased levels of female hormones.
Infections (<1%)
Viral infections can cause acute pancreatitis in persons with any age group, however this cause is more often seen in children. There are a host of viruses responsible like mumps, Epstein-Barr, coxsackie, varicella-zoster, and measles. These cases of acute pancreatitis tend to be milder when compared to biliary or alcohol-induced pancreatitis.
Bacterial infections can also cause acute pancreatitis & organisms include Mycoplasma pneumoniae, Salmonella, Campylobacter, and Mycobacterium tuberculosis.
Worldwide, ascariasis is a recognized cause of pancreatitis resulting from the migration of worms in and out of the duodenal papillae. Pancreatitis has been associated with AIDS; however, this may be the result of opportunistic infections, neoplasms, lipodystrophy, or drug therapies.
Hypercalcemia
Hypercalcemia means increased blood levels of calcium. There are various causes of having high blood calcium levels. This triggers or activates the pancreatic enzymes before they are secreted in the intestines and leads self- destruction of pancreas & an attack of acute pancreatitis. The treatment involves control of calcium levels along with treatment of pancreatitis.
Drugs (approximately 2%)
Considering the small number of patients who develop pancreatitis compared to the relatively large number who receive potentially toxic drugs, drug-induced pancreatitis is a relatively rare occurrence probably related to an unknown predisposition. Fortunately, drug-induced pancreatitis is usually mild. There are many drugs that have been reported to cause acute pancreatitis in isolated or sporadic cases.
Drugs definitely associated with acute pancreatitis include azathioprine, sulfonamides, sulindac, tetracycline, valproic acid, didanosine, methyldopa, estrogens, furosemide, 6-mercaptopurine, pentamidine, 5-aminosalicylic acid compounds, corticosteroids, and octreotide.
Drugs probably associated with acute pancreatitis include chlorothiazide and hydrochlorothiazide, methandienone, metronidazole, nitrofurantoin, phenformin, piroxicam, procainamide, colaspase, chlorthalidone, combination cancer chemotherapy drugs (especially asparaginase), cimetidine, cisplatin, cytosine arabinoside, diphenoxylate, and ethacrynic acid.
Very rare causes include diseases like vasculitis that can predispose patients to pancreatic ischemia, especially in those with polyarteritis nodosa and systemic lupus erythematosus. Also Exposure to toxins like organophosphate insecticide or scorpion sting can cause of acute pancreatitis.
Idiopathic
This is a loosely applied term used by doctors to mean “the cause is specific to an individual person” – in other words the cause is not known for certain. Many patients initially diagnosed as ‘idiopathic’ turn out to have a known cause – such as tiny gallstones or microliths missed by routine investigations. There are lots of other reasons for an initial diagnosis of idiopathic pancreatitis such as certain types of drugs, for which there is no convincing evidence.
Patients with idiopathic acute pancreatitis pose a problem because if the specific cause is not known, then no specific treatment can be given. In this case, it is important that the search for a cause should be thorough. These patients require a battery of investigations, which are done sequentially over a period, ruling out initially the common causes and those causes, which are indicated by the complete clinical picture. Only when common causes are ruled out tests are done for remaining. This is at times a tedious, time consuming, expensive process and tests the patience of patient & doctor alike. Ultimately, the doctor has to at time guess as to the likely cause (gut feeling) and advise the patient appropriately or council accordingly.
The pancreatitis can begin in children or young adults and is referred to as juvenile-onset idiopathic pancreatitis. Alternatively it may first begin in older adults and is referred to as late-onset idiopathic pancreatitis.
Genetic Changes
There may be a genetic basis to the pancreatitis. This often involves an alteration to a gene called SPINK-1 or an alteration to a gene called the cystic fibrosis gene, which is also called the CFTR gene. Inheritance in pancreatitis is explained in more detail below
Does Acute Pancreatitis Run In Families?
In general, the answer is NO. Because acute pancreatitis is common and there are many causes of this, simply by chance two or more members of a family may suffer from acute pancreatitis. For example, it would not be surprising if a mother and her adult daughter both developed gallstones and that both developed an attack of acute pancreatitis. Nevertheless rarely pancreatitis can run in families and falls into two types: hereditary pancreatitis and some forms of idiopathic pancreatitis.
Inherited Pancreatitis
Inherited pancreatitis occurs because they have an altered gene, which predisposes to pancreatitis.
What are genes?
Each person has exactly the same number of genes as every other person. The total number of genes is 30,000. Genes are in the nucleus of each cell of the body. Genes are like the blueprints in a factory. These blueprints (or genes) enable the cell to make proteins which then organize the two other types of basic molecule (carbohydrates and fats) to create particular types of cell and hence the different organs (such as liver, arms and legs and so on).
In the cells of different organs only some of the 30,000 genes in the nucleus are selected for use. This number varies from 6,000 to 10,000 genes in any particular cell. The different combination of genes used as blueprints for making proteins is how the human body can be organized in such a complicated way (compared to a simple worm that has only 900genes).
Genes are always in pairs, so that one set comes from the mother and one set comes from the father. There are tiny variations in each gene. These tiny variations are essential to make every person an individual. Occasionally a tiny variation in a gene can give rise to a disease condition.
What is mutation?
An alteration in a gene that gives rise to a disease is often referred to as a mutation (this is a Latin word that simply means ‘changed’). Patients and their families with inherited pancreatitis require the care of a specialist surgeon, pediatrician or gastroenterologist and genetic counseling.
Hereditary Pancreatitis
In this type of inherited pancreatitis there is a tiny variation in the cationic trypsinogen gene.
What are trypsinogen gene and its function?
The trypsinogen gene provides the blueprint to make a protein called trypsinogen. Trypsinogen is not active in any way and it is quite harmless. During a meal trypsinogen is secreted into the main pancreatic duct and then into the duodenum. Trypsinogen is then made very active by the removal of a protective cap at one end of the molecule. Once this cap has been removed it is now called trypsin, which is also an enzyme and is now very active. Trypsin is used to digest the proteins in foods such as meat.
What goes wrong in hereditary pancreatitis?
What happens in hereditary pancreatitis is that the protective cap of trypsinogen is removed in the pancreas. This unfortunately results in active trypsin in the pancreas. This activation occurs before it has had a chance to be secreted into the duodenum. This activated trypsin then begins to attack other proteins actually within the pancreas and causes acute pancreatitis. Affected individuals tend to develop pancreatitis as children, adolescents or young adults. There may be other members of the family with sugar diabetes.
The gene is officially called the PRSS1 gene and the two commonest alterations (or gene mutations) are called R122H and N29I. There are however 20 or so different mutations that have been discovered.
Does every family member get affected (penetrance)?
Not all members of the family will be affected in the same way. On average only half the individuals will carry the altered gene. The altered gene can be passed on by either the father or the mother and only one altered gene needs to be passed on to cause pancreatitis. The technical term for this kind of inherited disease is autosomal dominant. (‘Autosomal’ refers to the fact that is not linked to the sex genes and ‘dominant’ means that the altered gene is stronger than the normal gene). This means that half the children of an affected parent will have the gene passed on to them. Even then, some members of the family (about 20%) with the altered gene will not be affected at all. We call this 80% penetrance because the disease will only ‘penetrate’ into 80% of people with altered gene.
Is there any test for gene mutations in acute pancreatitis?
The presence of the gene can be tested for by a single blood test. Genetic counseling is required before any tests can be performed. Some families with hereditary pancreatitis have a normal set of PRSSI genes. This means that another gene is affected and scientists are trying to find out Which one this is.
Idiopathic Pancreatitis
Up to half of all patients with idiopathic pancreatitis (see above) have inherited one of two other altered genes that can trigger pancreatitis. One is called SPINK-1 and the other is called CFTR.
In order to protect the pancreas against accidental conversion of trypsinogen to trypsin, humans have been equipped with a safety mechanism called SPINK-1. This is a special enzyme that destroys any active trypsin in the pancreas and hence stops pancreatitis from occurring. Unfortunately some individuals have an alteration in SPINK-1 (N34S mutation), which destroys the safety mechanism.
About one in fifty people have this mutation but less than 1% of these people ever get acute pancreatitis. In other words this altered gene has less than 1% penetrance, or very low penetrance. This means that there is some other reason as well for the pancreatitis. This means that even though this mutation was inherited from either the mother or the father, the parents are usually not affected. Also this means that the disease is very unlikely to be passed on to the children even though there is a fifty-fifty chance that this mutation will be passed on to them.
Some patients have an alteration in the gene that causes cystic fibrosis, known as the CFTR gene. This gene provides the blueprint that makes a protein also called CFTR. This protein regulates the passage (or conductance) of small molecules through the outer surface (or membrane) of the cell. An alteration in both genes (the one from the mother and the one from the father) causes the disease called cystic fibrosis. For all of these reasons the full name of the gene is the cystic fibrosis transmembrane conductance regulator gene.
One in 20 of the normal population has a CFTR gene mutation but only a tiny handful has idiopathic pancreatitis. Individuals with cystic fibrosis disease have both of the CFTR genes altered. People with idiopathic pancreatitis only have one CFTR gene mutation (either from the mother or from the father). This type of genetic disease is therefore called autosomal recessive. We do not understand why some people with only one CFTR gene mutation develop pancreatitis. Scientists are trying to find out why this happens.
In these rare forms of pancreatitis, the symptoms begin as acute pancreatitis and usually progress to chronic pancreatitis. Most patients are actually never investigated for these rare causes for want of facility, lack of knowledge or awareness and high cost of investigations. They directly come to pancreatic surgeon with full- blown chronic pancreatitis. This also applies to a number of other causes of acute pancreatitis but gallstones never cause chronic pancreatitis.
Severe Pancreatitis And Its Complications
We do not know why some patients develop severe pancreatitis. Once this occurs, then the chances of complications and death are quite high. Hence it is important that specialists look after patients with severe pancreatitis if this is at all possible. They include pancreatic surgeon, gastroenterologist, intensivist & interventional radiologist.
Severe pancreatitis places a stress on all the main organs of the body: the heart, lungs, kidneys, other gut organs, the brain and the peripheral vasculature (the blood vessels that nourish all the organs). Patients who are elderly are less capable of coping with these stresses.
Equally, for reasons we do not understand, some young people also cannot cope with the stresses and death will occur despite every effort on the part of those caring for them.
What Are The Symptoms & Signs Of Acute Pancreatitis?
The cardinal symptom of acute pancreatitis is abdominal pain, which is characteristically dull, boring, and steady. Usually, the pain is sudden in onset and gradually intensifies in severity until reaching a constant ache.
Most often, it is located in the upper abdomen, usually in the epigastric region, but it may be perceived more on the left or right side, depending on which portion of the pancreas is involved. The pain may radiate directly through the abdomen to the back or left shoulder. May be worse within minutes after eating or drinking at first, especially if foods have a high fat content.
Nausea and vomiting are often present along with accompanying anorexia. Diarrhea can also occur. Positioning can be important, because the discomfort frequently worsens with the patient in the flat position.
The duration of pain varies but typically lasts more than a day. It is the intensity and persistence of the pain that usually causes patients to seek medical attention.
Atypical acute pancreatitis may be misdiagnosed and patients may come with various cardiac, pulmonary, hepatic, renal, abdominal, and metabolic disturbances.
Other symptoms that may occur with this disease include inability to pass wind or stools, gaseous abdominal fullness, hiccups, indigestion, mild yellowing of the skin and whites of the eyes (jaundice) & bloated tummy.
The doctor will 1st obtain a detailed history & perform a physical examination, which may show that you have abdominal tenderness or lump (mass), fever, low blood pressure, rapid heart rate, rapid breathing (respiratory) rate.
ALL PATIENTS WITH SUSPECTED ACUTE PANCREATITIS ON HISTORY & EXAMINATION ARE ADMITTED IN THE HOSPITAL FOR FURTHER MANAGEMENT.
The history may have to be revisited once acute pancreatitis is confirmed on investigations, to detect possible cause like alcohol, gallstone disease, drugs, viral illness, and subtle trauma etcetera.
Laboratory tests will be done. Tests that show the release of pancreatic enzymes include increased blood amylase level & increased blood lipase level. Other blood tests done in the acute setting include Complete blood count (CBC), Comprehensive metabolic panel including electrolytes, creatinine, BUN, liver function tests (bilirubin & liver enzymes). X-ray of chest & abdomen is performed to rule out intestinal perforation & obstruction. An USG (ultrasonography) of abdomen is obtained immediately.
When Do You Need a CT Scan?
A CT scan or MRI may be obtained if USG does not provide required information or in later course of disease if patient doesn’t improve or actually deteriorates. CT scan is also done by 5th or 7th day of illness if severe pancreatitis is suspected. Severity & prognosis can be assessed on CT scan.
Which Other Tests Are Done?
Once pancreatitis is confirmed on blood investigations, immediately tests to detect the cause are done. These include Liver Function Tests, blood levels of cholesterol, triglyceride, calcium & USG of abdomen. Certain blood tests, which help in patient management, are also done & include arterial blood gases, levels of C- reactive protein, procalcitonin & LDH. Many of these tests are repeated in next few days to follow the course of disease and detect signs of improvement or deterioration. In case of severe pancreatitis this is quite frequent and expensive too.
If cause of pancreatitis is not clinched in routine history & investigations, then patient may need more work up which is usually done after patient settles from current attack. These investigations will include ERCP / MRCP / EUS for imaging of biliary & pancreatic ducts & tumors, blood tests for viral markers, tumor markers, hormonal levels, immune system disorder, drugs & genetic studies for mutations.
How Soon Mild Pancreatitis Settles?
Patients with mild pancreatitis are treated with simple intravenous fluids & supportive treatment like rest to the bowel (patient is starved), painkillers, antiemetics, drugs that reduce gastric acid secretion & sometimes antibiotics. Patients usually recover over 3-5 days and are fit to be discharged by 7 -10 day.
How Is Severe Pancreatitis Treated?
At first, patients will be transferred to a High Dependency Unit (HDU) for intensive monitoring and given intravenous fluids and oxygen by mask. If the cause is due to gallstones, an ERCP and endoscopic sphincterotomy may be performed. Most patient’s recover but some require to be transferred to an Intensive Therapy Unit (ITU). This is necessary for assisted ventilation of the lungs and to treat kidney failure by hemofiltration or dialysis if needed. Some patients may need assist ventilation for longer duration & they need a special airway called tracheal tube inserted directly into the trachea (part of airway below the voice box) & the procedure is called tracheostomy. These patients also need special access to veins in the neck called jugular lines for giving medications, fluids & nutrition.
Keeping your weight up during the illness can be very difficult. At all times you will be encouraged to eat by mouth and drink what fluids you can. You will be seen by the nutritionist who will advise on other ways to improve your calorie intake. This includes the insertion of an NG tube into the stomach (naso-gastric tube) and giving you a continuous liquid diet down this tube. If you are unable to tolerate the NG tube a narrow tube will be inserted into the small bowel (jejunum) using a flexible endoscope. This is like regular endoscopy and is done with local anesthetic spray to the back of the throat and intravenous sedation. The tube is called an NJ tube or naso-jejunal tube and the feeding with a liquid diet slowly dripped in using this tube is called naso-jejunal feeding. If patient is undergoing surgery, then the feeding tube will be inserted directly into a jejunal (small intestine) loop directly & brought out through skin. This tube is used for feeding & is called feeding jejunostomy. This avoids the discomfort of nasal tube for the patient but is not devoid of complications.
Sometimes extra feeding has to be given straight into a vein and is called parenteral feeding. This can be done by inserting a long catheter (tube) into a vein in one of the arms and then the tip is pushed into one of the large veins close to the heart (this is called a PIC line). If the arm veins are collapsed then a catheter will need to be pushed into one of the neck veins and then the tip is pushed towards the large veins near the heart. This is sometime called TPN or total parenteral nutrition.
Once you are over the worst of the worst of the severe pancreatitis but you are still unable to keep your weight up despite eating some food by mouth you may be fed with a PEG tube (percutaneous endoscopic gastrostomy). A PEG tube is inserted using a flexible endoscope, inflating the stomach with air and pushing a guide wire through the skin into the stomach. A permanent feeding tube is then passed over the guide wire into the stomach. With a PEG tube you can eat and drink as much as you feel like. Any extra calories can then be given using a liquid diet dripped into the PEG tube. You may well be sent home with the PEG tube still present.
Pancreatic Necrosis
One or more CT or MRI scans will be necessary to assess the state of the pancreas during the course of disease. There may be severe death of the tissue (necrosis) of the pancreas or tissues surrounding the pancreas. It is common to see one or more acute fluid collections in the abdomen. These are usually quite harmless and disappear without specific treatment.
Only the CT or MRI can reliably show whether there is pancreatic necrosis (or gangrene of the pancreas). This usually does not fully appear until a week or so after the start of the illness. If there is necrosis it is important to know whether this is infected (called infected pancreatic necrosis) or not infected (also called sterile pancreatic necrosis). Infected pancreatic necrosis is similar to wet gangrene (and needs urgent removal) and sterile pancreatic necrosis is similar to dry gangrene (and usually improves without specific removal).
It is not always possible to tell from the CT or MRI whether the pancreatic necrosis is infected or not. The best way to do this is by inserting a needle into the dead pancreas and removing some tissue for inspection for bacteria and fungi. A very fine needle is passed into the pancreas using CT and the dead tissue sucked up (or aspirated) into a syringe. The procedure is therefore done in the X-ray department. The samples are examined under the microscope but it is usually difficult to see the bacteria and /or fungi. Therefore these are also cultured in the microbiology department. This means that the results may not be available for 24 hours or so. This procedure is known as fine needle aspiration for bacteriology and fungi, or FNABF. Most patients with extensive pancreatic necrosis will have FNABF performed at least once. Some patients will need this to be done two or more times (usually at weekly intervals) before the doctors are sure whether there is infection or not. Infection in necrosis can change the line of treatment; hence it is important to rule out infection at every step.
If the necrosis is extensive or if there is evidence of infection of the necrosis, then surgery will be needed. The timing of the surgery and the extent of surgery are difficult decisions to make even for experienced pancreatic surgeons. Once it is decided to operate, the likelihood of success is anywhere between 20% and 80%, but this depends very much on individual cases. The procedure used for removing extensive pancreatic dead tissue (necrosis) is called a ‘necrosectomy’. The procedure may be performed as a conventional open operation or may be done using less invasive ways like laparoscopy
Open Necrosectomy:
This requires a large open operation to remove dead pancreatic tissue. Operation is done under general anesthesia. For several weeks (or longer) tubes are left behind for continuous wash out of small pieces of dead tissue (lavage). More than one operation may be necessary over a period of few weeks.
Minimally Invasive Necrosectomy:
It may be possible to remove dead pancreatic tissue using “keyhole” surgery. The advantage is that the success rate may be better in very ill and elderly patients compared to open necrosectomy. This involves inserting a guide wire into the pancreas necrosis using CT in the X-ray department (see picture). The patient is then taken to the operating theatre where a telescope is introduced along the guide wire into the pancreatic necrosis. The dead tissue is removed. As with open necrosectomy a large tube is left in the middle of the dead pancreas for continuous washout. This procedure is often referred to as ‘skunking’. This procedure can often be done using local anesthetic and mild sedation and usually has to be repeated several times. It is only available in a few specialized centers.
The process of clearing all of the pancreatic necrosis can be very time consuming and may take weeks or months. It is very expensive too. Hence it is important that you remain patient. In order to discharge patients as soon as possible it is likely that the drainage tube will still be present when you go home. You will be seen regularly in outpatients and the tube will slowly be shortened before it is finally removed.
Failure to survive a severe attack of acute pancreatitis despite all the treatment on ITU and surgery is due to the inability of the different organs to cope with the stress of acute pancreatitis. In young people, even though the heart and lungs respond to drugs and ventilation and the kidney function is replaced by dialysis, the peripheral vasculature becomes unresponsive to drugs. The blood pressure then falls and it becomes impossible to keep the patient alive. On the whole, most patients tend to survive an attack of severe acute pancreatitis although this may take several months of treatment in hospital & massive expenditure. Despite an overall improvement at a later stage, localized complications may develop, which are principally a pseudo cyst or an abscess (see below).
What Are Complications Of Pancreatitis?
Splenic Vein Thrombosis
A thrombus simply means blood clot. In severe necrotizing pancreatitis it is quite common for the splenic vein to become blocked off because of a clot. This is because the pancreatitis irritates the splenic vein to cause the clot. Once the pancreatitis is cured the clot is usually dissolved normally by the body. Sometimes however the clot and blockage of the splenic vein becomes permanent and you are now at risk of venous bleeding (bleeding from the system of veins). The treatment of venous bleeding is described below.
Portal Vein Thrombosis
This is an unusual complication of severe necrotizing pancreatitis. The pancreatitis irritates the portal vein to cause a clot. There is a risk that the clot and blockage of the portal vein will become permanent and cause venous bleeding (bleeding from the system of veins) or a build of fluid in the abdomen (ascites). The treatment of venous bleeding and ascites is described below.
It may be possible to clear the clot (also called a thrombectomy) in the portal vein using a procedure performed in the X-ray department. Usually using local anesthetic (but sometimes requiring a general anesthetic) a wire is pushed through the skin and into one of the branches of the portal vein within the liver. The guide wire is then advanced towards and through the blood clot. A special miniature wire basket is then used to try and retrieve the blood clot. The full name of this procedure is percutaneous trans hepatic portal venous thrombectomy or just percutaneous thrombectomy.
If this is not successful then it may be possible to insert a tube through the clot to keep the vein open using the same guide wire. This is known as percutaneous trans hepatic portal venous stenting or just percutaneous venous stenting. If stenting is successful then your doctors may decide to give you long term aspirin (which prevents the platelets that cause a clot from sticking together) or warfarin (which keeps the blood thin). There is a special way of checking if there is blood flow through the portal vein using ultrasonic waves (similar to that used by submarines). This test is called duplex scanning and is performed in the X-ray department. This is similar to a normal ultrasound examination.
Venous Bleeding
If there is permanent splenic vein thrombosis and/or portal vein thrombosis then the blood pressure will build up in the tiny vessels that normally drain into these big veins. The tiny veins now become much larger and are called venous collaterals. These slowly increase in size over some months or years and become tortuous. These are then referred to as varices (similar to varicose veins in the legs, but now inside the abdomen). The varices may appear in the stomach and in the lower gullet. There is a small but real danger that bleeding may occur from rupture of one of these varices. For this reason it is important that you maintain close contact with your consultant in out-patients. From time to time the consultant will organize for you to have an endoscopy of the gullet and duodenum to see if the varices have enlarged. If the varices are large then they can be injected with medicines called sclerosing agent, using the endoscope – this is called endoscopic sclerotherapy (EST) or ligated using special endoscopic bands – this is called endoscopic variceal ligation (EVL).
If bleeding does occur you will need to come to hospital as an emergency – usually there is vomiting of blood. In this situation you will be admitted to ICU, given intravenous fluids & blood transfusion. You will also be given injections or a continuous infusion of special drugs that will reduce the pressure in the varices. This will then be followed by endoscopic sclerotherapy. These measures are usually successful.
Very occasionally the bleeding will keep recurring and in this case surgery is required. The operation will involve removal of the spleen and disconnection of the varices from the stomach. This operation is called gastric devascularisation and splenectomy.
Occasionally a stent is introduced across the hepatic and portal veins (TIPSS) draining the blood from portal circulation into main system thereby decreasing blood pressure in varices and stops bleeding.
Arterial Bleeding
During the course of severe necrotizing pancreatitis about one in fifteen patients will develop some type of bleeding from a small or large artery. This may even occur during skunking – and since you would be awake, this may seem quite alarming. This can sometimes happen during the natural course of severe pancreatitis because the pancreatitis causes an irritation and erosion of the outer wall of an artery near the pancreas.
Sometimes this may cause a pulsating sac to be created next to the artery. This is called pseudo aneurysm (pronounced ‘Sue-doe an-new-rism’). This is very likely to bleed with serious consequences. In either case it is important to block off the small gap in the artery responsible. Your doctors are however always prepared for this.
If this does occur whether you are in the ward, in HDU or in ITU you will be taken immediately to the X-ray department. You will be placed on an X-ray table, the skin cleansed with antiseptic and covered with sterile gowns. Under local anesthetic a tube will be inserted into the artery in either the left or right groin (called an arterial catheter). ‘Dye’ (or contrast) is then injected into the catheter to see where it goes using an X-ray television screen. The catheter can be guided to the exact place where the bleeding is taking place (this is called selective arteriography). The bleeding will then be stopped by injecting special metal coils and glues into the catheter (this is called embolization). The whole procedure is called selective arterial embolization and is highly successful. Arterial embolization can sometimes result in decrease or stoppage in blood supply of small or large segment of intestine supplied by it. This can cause perforation or gangrene of the intestine and would require a surgery for the same.
Only rarely is it necessary to try to stop the bleeding with open surgery and is only performed if the selective arteriography has not identified the source of bleeding or if the selective arterial embolization has failed.
Colonic Necrosis (Gangrene Of Large Intestine)
On rare occasions in severe necrotizing pancreatitis, the pancreatitis spreads into the base of the large bowel (also called the colon) and cuts some of its blood supply off altogether. This will cause the death (or necrosis) of that part of the colon – hence colonic necrosis.
The patient will become very sick and there may be a large amount of bleeding. In this case emergency surgery is needed to remove the dead colon. At the time it may be necessary to avoid joining the bowel ends together. In this case one or both ends of the bowel are brought out onto the skin as a colostomy. Closing of intestine would be done at a later time when the patient has recovered from the pancreatitis altogether.
Like large intestine, patient with severe panreatitis can rarely develop gangrene and perforation of duodenum and small intestine also.
Pancreatic Fistula
The term ‘fistula’ is an old medical term meaning an abnormal connection between one surface and another. When there is a connection between the pancreatic duct and the skin this is known as an external pancreatic fistula. This happens naturally as part of the treatment of most patients with extensive pancreatic necrosis.
Most pancreatic fistulas dry up with no special measures except that the drainage tube is shortened slowly over many weeks before it is finally removed. Only in exceptional circumstances is it necessary to encourage closure of the fistula by pancreatic stenting or the use of octreotide injections to reduce pancreatic secretions. Sometimes a surgery is required for external pancreatic fistula. The surgery may involve joining an isolated segment of intestine to the fistula tract – Fistulojejunostomy, or removal of portion of pancreas— pancreatectomy.
Pseudocyst
(Pronounced ‘Sue-doe-cyst’) This is a cystic (filled with liquid) swelling which lies in the pancreas or next to the pancreas and which contains high concentrations of pancreatic enzymes. Often pseudo cysts disappear without any specific treatment. If a pseudo cyst remains or enlarges, it may cause nausea, vomiting, pain and weight loss, in which case, treatment is necessary.
There are different ways to treat large pseudo cysts. Sometimes it is possible to insert a tube into the pseudo cyst under local anesthetic in the X-ray department and drain the fluid away without surgery. This is called external drainage or percutaneous drainage. The pseudo cyst can be drained internally by endoscopic stenting. Often the most appropriate method is by surgery. The operation of Roux-en-Y pseudocyst-jejunostomy drains the pseudo cyst into a specially created small bowel channel. The operation of pseudocystgastrostomy drains the pseudo cyst into the stomach.
Pancreatic Abscess
A collection of pus may develop in or near the pancreas during or after an attack of severe pancreatitis. The treatment is usually successful and just requires external drainage (or percutaneous drainage) with a tube inserted under local anesthetic in the X-ray department but may occasionally require open drainage surgery.
What Can I Eat?
For a few weeks after an attack of acute pancreatitis you should eat at regular intervals. It is usually better to take four or five snacks a day than a full meal. (MULTIPLE SMALL MEALS) If you have gallstones, and for some reason your gall bladder has not been removed, avoid fatty foods such as butter, eggs, fried foods, sausages and bacon. Following removal of your gall bladder you are free to eat anything you wish. You will have a very healthy appetite and you may put on more weight than you would otherwise, unless care is taken to avoid excess calories.
If you have had extensive pancreatic necrosis it is likely that you will need pancreas enzyme supplements (see below) and even insulin if you have developed sugar diabetes (see below).
Can I Drink Alcohol?
Alcohol is not recommended for patients who have recurrent acute pancreatitis and should be avoided in patients for whom the cause of their acute pancreatitis is alcohol. Alcohol must also be avoided in patients with idiopathic pancreatitis or hereditary pancreatitis. If alcohol is not the cause of your acute pancreatitis you may drink alcohol if you wish.
A unit of alcohol is 100mls of 10% alcohol (by volume) equivalent to a half-pint of regular beer or lager, a regular glass of table wine. The recommended intake for healthy adults should be no more than 21 units per week for women and no more than 28 units per week for men.
Living Without A Pancreas
There are some patients who have had either their pancreas removed or who still have pancreatic tissue but which is not functioning at all. Both types of patient are perfectly able to lead a normal life provided they take regular enzyme supplements and insulin injections.
Pancreatic Enzyme Supplements
There are many preparations available. These preparations differ considerably in their effectiveness of action. The better preparations consist of capsules containing scores of small granules.
The enzyme preparations can also be divided into two types depending upon their strength of action: regular and high dose. The capsules need to be taken during each meal and with any snack. Requirements vary enormously from patient to patient: typically 20-30 high-dose capsules per day are required but this can be lower or much higher. The requirements vary greatly from patient to patient partly because of the different level of secretion by any functioning pancreas and partly because there are still some enzymes secreted by the salivary glands, tongue, stomach and small intestines but which also varies greatly from person-to-person.
In a few cases of children and adults with cystic fibrosis, a serious problem with the large bowel (colon) has been reported. This condition is called fibrosing colonopathy and causes narrowing of the bowel. It seems to be related to the use of a particular acid-resistant coating of the enzyme preparations (called methacrylic copolymer). The problem does not arise with preparations without this covering. The latter preparations are therefore recommended. The ingredients are always listed on the pack leaflet or label. Once patients are accustomed to taking enzyme supplements, they are usually allowed to adjust the number they take themselves to suit their own individual needs
Insulin
There are many types of insulin available including human insulin obtained by genetic engineering. Precise dosing and frequency of injections is an individual matter. Being under the care of a diabetic specialist is obviously important in the first instance.
Gastric Acid Suppressing Tablets
Medication of this sort is often prescribed to be taken once or twice a day. Pancreatic juice normally counters the acid of the stomach. In the absence of the pancreas, there may be excess acid which can cause dyspepsia.
There is also some evidence that taking this type of medication helps the action of pancreatic enzyme supplements which means that fewer capsules are required each day.
Living Without A Spleen
Pancreatic surgery sometimes necessitates removal of the spleen. This is much more of a problem in children than in adults. Without the spleen there is a small but real risk of developing a serious infection caused by certain bacteria especially pneumococcus. All children and adults without a spleen therefore require regular pneumococcal vaccination. All patients should also receive vaccination for meningococcus groups A and B, and children less than 4 years old require Hemophilus influenza type b vaccination. Children will also need to take a daily antibiotic. The risk is much less in adults, but nevertheless daily antibiotics are usually prescribed. Nevertheless if any infection develops, then appropriate antibiotics (such as penicillin or erythromycin) must be taken over-and above any other types of antibiotic that are required.
Removal of the spleen sometimes causes the number of platelets in the blood to increase. This increases the risk of developing unwanted blood clots. Regular blood tests are therefore needed. If the number of platelets in the blood rises excessively, it is common practice to prescribe low dose aspirin which reduces the risk of undesirable clotting.
Above information will help you to make an informed decision but it cannot replace the professional advice and expertise of a doctor who is familiar with your condition. You may have questions that are not covered; you should discuss these with your surgeon. You must remember every individual is different.
Doctors Dealing With Pancreatic Disease That You May Meet
Dietician: This is a specialist who is not a doctor but is an expert in advising on various types of diet.
Endocrinologist: A physician who is highly specialized in glandular problems including sugar diabetes.
Endoscopist: This may be a gastroenterologist or a surgeon who is able to undertake endoscopy (examination of the stomach or bowel using a flexible telescope). A few endoscopists can also perform ERCP and EUS, which are specialist forms of endoscopy that examine the biliary and pancreatic ducts and the pancreas
Gastroenterologist: A physician who is highly specialized in ‘gut’ problems and is also usually an ‘endoscopist’.
General physician: A consultant medical doctor who works in a hospital and who is broadly specialized including ‘gut’ problems.
General surgeon: A consultant surgeon who works in a hospital and who is broadly specialized including ‘gut’ problems.
Geneticist: A consultant who specializes in diseases which may be inherited and may be able to provide additional help to that normally given by your other specialist doctors.
Nutrition team: A team of specialist doctors and nurses involved in providing specialist nutritional support, including the insertion of venous access lines and special stomach tubes to help patients who are unable to eat properly.
Pediatrician: A consultant who specializes in the care of children and who may be called to investigate a pancreatic problem in young children or teenagers.
Pain team: A team of specialist doctors who specialize in providing special treatment measures and support for patients who are experiencing difficulties in pain control.
Radiologist: A consultant who specializes in taking X- rays and scans of various sorts at the request of other specialists.
Specialist surgeon: A general surgeon who is highly specialized – a so-called PB-specialist is a pancreato- biliary surgeon.
For Consultation Available At:
Timing: Monday To Friday - 9am To 5pm & Saturday 9am To 2pm
(Consultation Only by Appointment)
Address: Lilavati Hospital, A-791, Bandra Reclamation Rd, Bandra West, Mumbai, Maharashtra 400050
For Appointment call: 09821046391
Timing: Saturday 9am To 10am
(Consultation Only by Appointment)
Address: 93, ACI Hospital, 95, August Kranti Rd, Kemps Corner, Cumballa Hill, Mumbai, Maharashtra 400036
For Appointment call: 09821046391
Consultation Only by Appointment
Address: Raheja Rugnalaya Marg, Mahim West, Mahim, Mumbai, Maharashtra 400016

